Services
New ways of looking at the world create new opportunities for improved outcomes.
At Data Revolution, we see the person as a dynamic health trajectory from birth to death with a complex network of drivers.
Risk algorithms tell us where the person is on that trajectory and what drivers will steer it favourably in the next phase.
The following are examples of what we have developed and implemented in the past.
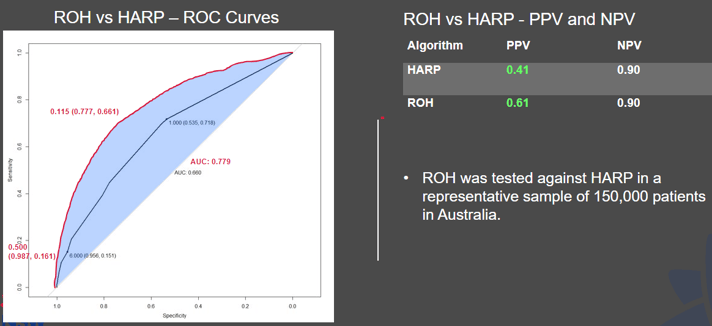
Risk of Hospitalisation (RoH)
RoH predicts a patient’s unplanned hospitalisation in the next 12 months, with 50% better predictive performance than *HARP.
*Hospital Admission Risk Prediction - Canadian built tool, used internationally to predict hospitalisation
Risk of Readmission (RoR)
RoR predicts a patient's unplanned readmission to hospital in weeks 5-12 post-discharge from an unplanned admission.
Our findings show that seeing your GP in the first week post-discharge cuts your risk of readmission by half in the subsequent 6-12 months period.
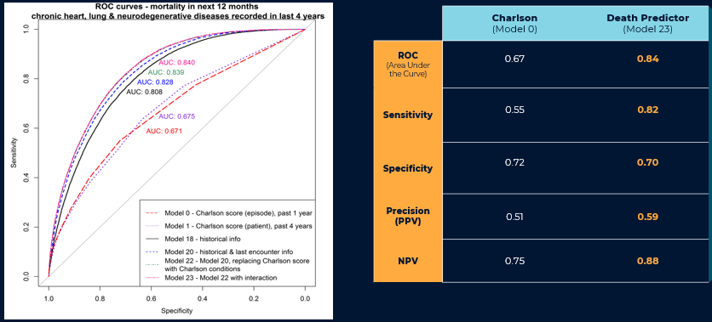
Death Risk Predictor (DRP)
DRP predicts a patient’s risk of death in the next 12 month for proactive provision of palliative care.
DRP shows 50% better predictive performance than *Charlson Comorbidity Index (CCI), the international standard.
Risk of Hospital Acquired Complications (RoHAC)
RoHAC predicts a patient's likelihood of having one or more of the 16 recognised complications affecting quality and safety in the hospital setting.
The fundamental premise that health determinants form a complex network lead us to the design and in-situ evaluation of population health programs where the whole of the health system is mobilised in coordination to improve health outcomes.
Objectivity in Science
One of the greatest practical challenges of this approach to healthcare is objective scientific evaluation 'after the fact', due to:
-
Complexity of the program and service model
-
Lack of a real-time control group for comparison
Learn how we overcome these challenges through data science in our PSM concept video.
Capturing and quantifying the network of health drivers creates opportunities for multi-disciplinary, multi-modal interventions which can achieve long lasting positive health outcomes and sustained socio-economic productivity.
From Reactive to Proactive
Currently, The ‘clinical’ mind is quite efficient in healthcare whereas the ‘integrating’ mind is often absent.
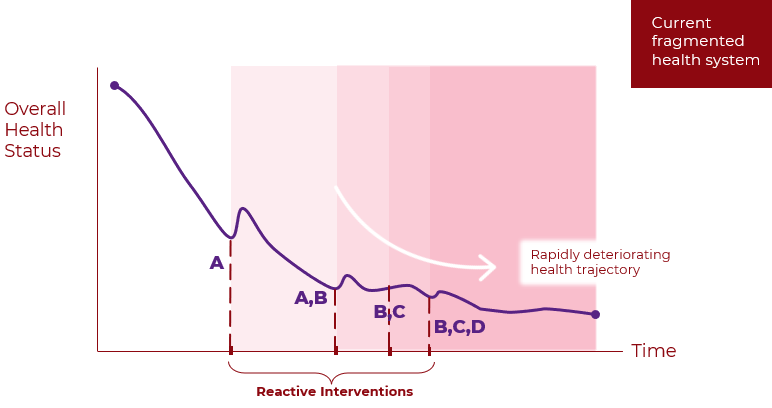
We are interested in finding the combination of interventions that most favourably alter the patient’s health trajectory.
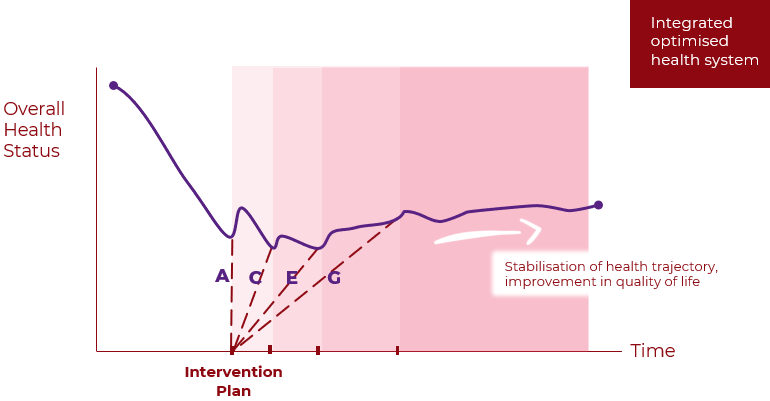
A practical example involving diabetes management is illustrated below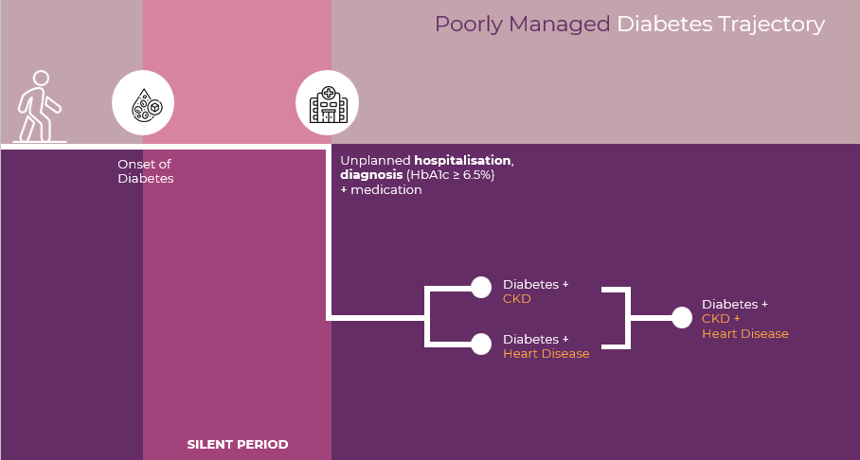
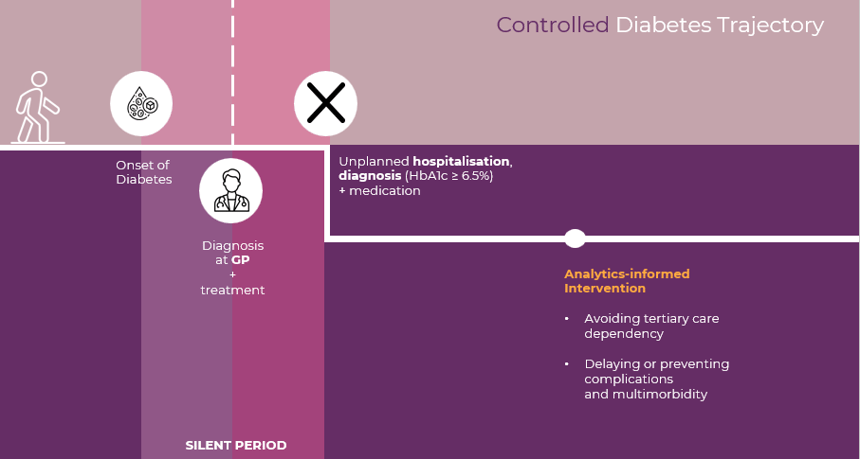
Just as we can capture the full network of drivers for health outcomes, we can quantify the benefit of a successful health program in relation to all modes of social investment.
This enables policy makers and institutions to fund, with confidence, interventions with maximal return on investment.
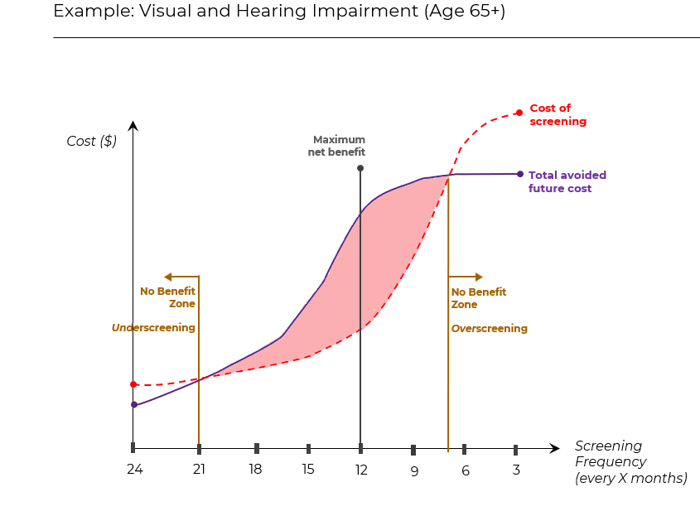
Cost-benefit Sweet Spot